Baylisascaris procyonis
Roundworms
Baylisascaris procyonis roundworms from raccoons can hurt or kill humans. The danger grows as more raccoons roam urban areas. Learn how to protect yourself, your kids and your pets, including rabbits.
Baylisascaris procyonis roundworms are a dangerous consideration if your rabbit shows evidence of brain inflammation such as stiffening in spasms or seizures, and has contact with the environment.
People sometimes ask: Are there rabbit sicknesses that people can get? It is as yet unclear whether B. procyonis roundworms can be transmitted directly from rabbits to people. But, if your rabbit becomes infested with the raccoon roundworm, then the chances are very great that raccoons and their roundworm-laden latrines may be closer to you than you’d like to think.
Symptoms in Humans
Inquisitive children are particularly at risk, since they tend to put things in their mouths.
Most cases of Baylisascariasis occur in children under 2 years old due to pica, geophagia (eating dirt), and lack of hand-washing, and many cases have been fatal. There had been roughly 20 documented cases of death or injury in humans through 2002. Once infected, permanent disability can occur, or death, over a period of roughly 1.5 - 2 years from the onset of the first symptoms.
In 2003, a screening of 389 children aged 1-4 years old in the Chicago region revealed that the immune systems of 31 kids (8%) had responded to a Baylisascaris infection but these kids were all asymptomatic at the time.
Check out this 2017 story of a Seattle toddler who became infected with baylisascariasis
Picture: Baylisascaris procyonis life cycle illustration, credit: http://cid.oxfordjournals.org/content/39/10/1484.full
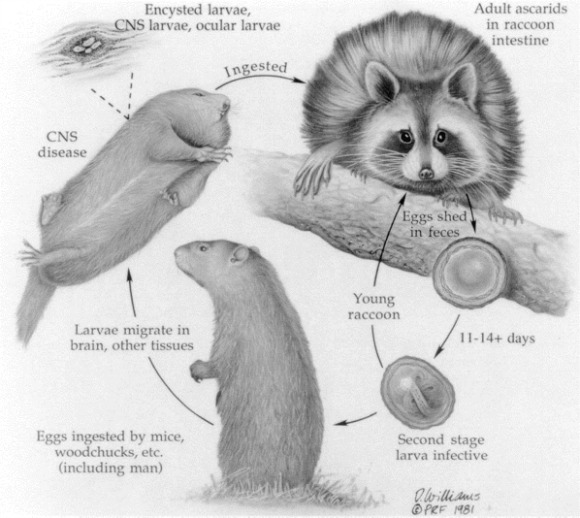
The screening of children in Chicago had been prompted by the discovery of 2 other youngsters in the area with severe brain disease due to Baylisascaris procyonis larval migration.
The neurological symptoms of baylisascariasis range the gamut from asymptomatic, to truly severe nervous system deficits, such as:
- Lack of balance, disorientation, agitation
- Lethargy, paralysis, permanent loss of function and disability
- Coma and death
Other symptoms depend on the affected area:
- Eyes: blindness
- Skin: rashes from larval migration
- Guts and muscles can also be affected, with weakness and other symptoms depending on the area of infestation
The symptoms occur gradually, confusingly, inexorably over months or a couple years until death overtakes the patient or the symptoms finally stabilize (with or without recovery of function). Human infection is still uncommon, but the possibilities are on the rise as the population of raccoons rises.
The Center for Disease Control now advises physicians everywhere to include baylisascariasis in their differential diagnoses whenever the symptoms and circumstances warrant.
The CDC states:
- "Human clinical infections are uncommon, probably because most persons do not have intimate contact with the sites or exhibit those behaviors (ingestion, pica, geophagia) that would result in heavy infection. Nonetheless, the potential for infection exists, especially for young inquisitive children who might exhibit such behaviors. Moreover, because of the widespread distribution of raccoons, as well as diagnostic difficulties and lack of clinical experience with the spectrum of disease caused by B. procyonis in humans, mild or subclinical infections likely go unrecognized. In fact, asymptomatic, low-level infection with B. procyonis is probably the most common form of infection" (http://wwwnc.cdc.gov/eid/article/9/12/03-0039_article.htm).
Therefore, “for any child who presents with eosinophilic meningoencephalitis and a history of possible exposure to raccoon feces, the possibility of B. procyonis infection should be strongly considered” (http://cid.oxfordjournals.org/content/39/10/1484.full).
In the words of the Oxford Journal:
- “B. procyonis infection should be considered in any patient, particularly a young child, with evidence of neurologic or ocular disease, and especially with eosinophilic meningoencephalitis in combination with peripheral blood eosinophilia and a history of possible exposure to raccoon feces. Such patients should be treated immediately with albendazole and steroids” (http://cid.oxfordjournals.org/content/39/10/1484.full).
Avoiding Baylisascaris procyonis Roundworm
Exposure and Infection in Humans
Discussions centering around human exposure to the raccoon roundworm continually mention the danger of raccoon latrines, around and within which are nearly unbelievable quantities or roundworm eggs if frequented by infected raccoons. That likelihood at any given latrine is greater than 50%.
- Recognize a raccoon latrine when you see one! Teach your small children to avoid raccoon latrines and to wash their hands carefully when they come inside.
- Immediately decontaminate any latrines. Protect yourself with gloves, overalls and rubber boots. Double-bag the scat and place in garbage can. If you found the latrine on the ground, include 2-3 inches (5 – 7.5 cm) of soil in the discard materials. Or burn the dung. Get the help of wildlife professionals if needed.
- Baylisascaris procyonis eggs can be destroyed with high heat, such as a propane torch, pressurized steam or boiling water. A bleach solution does not destroy the eggs, but it does render them less sticky, which may help to wash them away from surfaces which one cannot simply torch.
- If you know your child has been exposed to a raccoon latrine, and especially if you see him put scat in his mouth, he should immediately receive therapeutic doses of the antiparasitic albendazole and steroids. The raccoon feces should be examined for B. procyonis eggs. The cure rate for exposure to infective eggs within 3-10 days is 95+%. The key is early treatment.
- Periodically inspect your property for raccoon latrines, including the roofs, crotches of tree branches, on or under porches, and in and around landscaping, especially if you know raccoons are frequenting your neighborhood.
- Prevent toddlers from playing in areas known to have contained raccoons or their latrines.
- Stop feeding and/or attracting the raccoons. Don’t leave your dog and cat food outside where raccoons could help themselves. Feed birds from raccoon-proof feeders.
- Don’t keep raccoons as pets. At least one toddler died (in Minnesota) due to exposure to a pet raccoon.
- Enlist the help of wildlife experts in order to euthanize or relocate nuisance raccoons.
- If a pet rabbit, dog or cat becomes an intermediate host, this should alert you to the need to search, disinfect and destroy raccoon latrines and to protect your toddlers from exposure to Baylisascaris procyonis roundworms.
Learn more about the Raccoon Roundworm here
- https://www.michigan.gov/dnr/0,4570,7-350-79136_79608_85016-27261--,00.html
- http://cid.oxfordjournals.org/content/39/10/1484.full
- http://www.ag.ndsu.edu/pubs/ansci/animpest/v1227.pdf
- http://www.dnr.state.mn.us/livingwith_wildlife/raccoons/index.html
- http://www.dnr.state.mn.us/volunteer/janfeb02/fn_raccoon.html (may be offline)
- http://suite101.com/article/baylisascaris-procyonis-raccoon-parasite-a74870
- Roussere GP, Murray WJ, Raudenbush CB, Kutilek MJ, Levee DJ, Kazacos KR. Raccoon roundworm eggs near homes and risk for larva migrans disease, California communities. Emerg Infect Dis [serial online] 2003 Dec. Available from: http://wwwnc.cdc.gov/eid/article/9/12/03-0039.htm
Double-Value Guarantee
Our policy is to always OVER-deliver
on value,
which is why your purchase is fully covered by our
Double-Value
Guarantee.
Go ahead - take any of our e-books for a test drive. Peruse our detailed informational and educational e-books. Examine our plans for building rabbit cages, runs, or metal or PVC hutch frames. Check out the Rabbit Husbandry info e-books.
If you aren't completely satisfied that your e-book purchase is worth at least double, triple or even quadruple the price you paid, just drop us a note within 45 days, and we'll refund you the entire cost. That's our Double-Value Guarantee.
Note: When you purchase your
e-books, they will be in PDF format, so you can download them to any device that
supports PDF format. We advise making a back-up copy to a drive or cloud
account. If the books are lost, you can also purchase another copy from Raising-Rabbits.









New! Comments
Have your say about what you just read! Leave me a comment in the box below.